Genome sequencing and clinical trials are helping brain cancer patients in Hong Kong SAR to live longer. As Shadow Li reports, closer collaboration within the Greater Bay Area will turn the region into a world clinical trials hub.
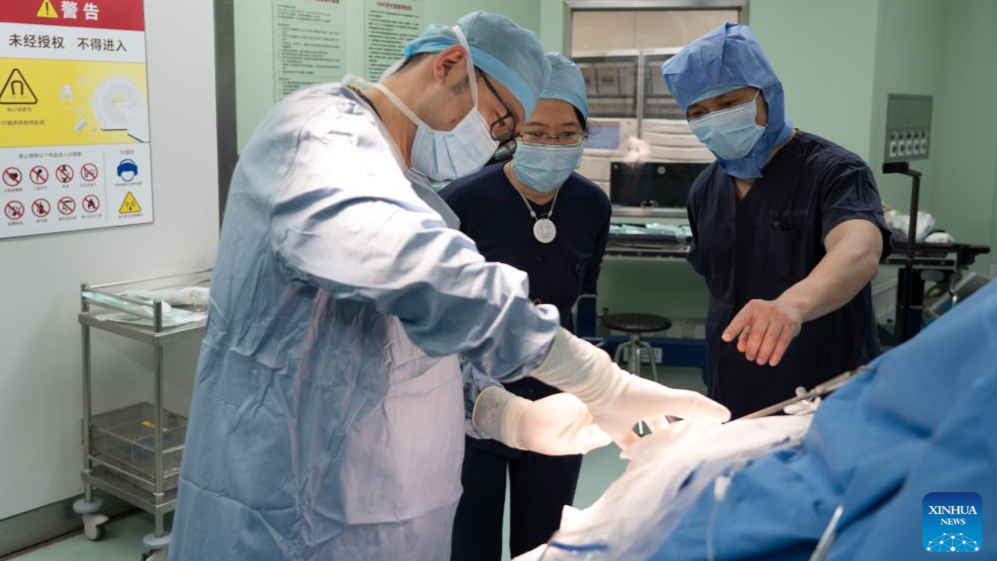
Glioblastoma — a malignant form of brain cancer — is among the deadliest diseases worldwide with patients under treatment given 12 to 15 months to live, or just four months for those not being treated.
But some Hong Kong patients are beating the odds.
Aya El Helali, a clinical assistant professor at the Department of Clinical Oncology of the University of Hong Kong, has seen a patient survive beyond five years, defying the disease’s typical survival rate of less than 10 percent. She credits this to combining genome sequencing with clinical trials.
Glioblastoma patients who’ve exhausted standard treatment methods are sequenced to identify mutations that may qualify them for clinical trials. They would then receive repurposed drugs or new therapies originally designed for other medical conditions before and after undergoing brain surgery.
READ MORE: HK’s genome project uncovers world’s new disease
Genome sequencing, conducted under the auspices of the Hong Kong Genome Institute, will confirm if the drugs prescribed for a patient can reach the tumor. “If it doesn’t, we’ll stop exploring it,” El Helali said on the sidelines of a rare disease conference last year. “If it does, we’ll take on more patients to effectively assess its impact on their rate of survival.”
Such a “fail fast” approach can determine a drug’s effectiveness on glioblastoma patients within one or two years, compared to five to 10 years in traditional Phase III clinical trials that often fail. “In which case, we would have missed the boat for another five to 10 years,” explains El Helali.
According to the seasoned oncologist, tumor sequencing has shown that some glioblastoma tumors are driven by the immune system. Without genomic screening, patients, historically, would not respond well to immunotherapy at trials. Sequencing now helps to identify specific mutations that make immunotherapy more effective, enabling some patients to live for five to seven years. Not all patients have this mutation, but for those who do, the right treatment can significantly prolong their lives.
She says the traditional “one-size-fits-all” approach has failed in combating glioblastoma. With genome sequencing, doctors can now refer patients to targeted therapy trials based on their mutations, enabling more precise treatment.
At present, Hong Kong records about 100 glioblastoma cases annually. In 2023 alone, 143 patients were diagnosed with the disease, according to the Hospital Authority.
El Helali says the core principle of the innovative treatment regime is to ensure that the right drug reaches the right patient and the tumor itself. This approach could be applied to other hard-to-treat types of cancer, like pancreatic, advanced breast, ovarian and lung that have stopped responding to treatment.
The initiative is being carried out in collaboration with the HKGI and the Greater Bay Area International Clinical Trial Institute — a Hong Kong Special Administrative Region government facility launched in 2024, where El Helali serves as an adviser.
El Helali says the “beautiful marriage” of the two medical institutes allows the SAR to work closely with local and overseas pharmaceutical agencies, helping glioblastoma patients in the Greater Bay Area to gain access to clinical trials from around the world.
The GBAICTI is strategically based at Hong Kong Park of the Hetao Shenzhen-Hong Kong Science and Technology Innovation Co-operation Zone — a pilot zone located between Hong Kong and southern Chinese mainland tech powerhouse, Shenzhen. Along with its mirror image Greater Bay Area International Clinical Trials Center (BAY TRIAL) across the river in Shenzhen Park, the twin organizations form the “one-institute, one-center” paradigm to spearhead the development of clinical trials in the region.
The institutional ambient makes Hong Kong a “superconnector” to bridge the gap for Chinese pharmaceutical companies to make their global forays, and facilitate international drugs entering the mainland in a clinical trial setting, El Helali envisions. She added that a number of international biopharmaceutical firms like GSK and Johnson & Johnson are planning to start clinical trials through GBAICTI.
“Our vision is to make the Greater Bay Area a world clinical trials hub by working with other cities in the region, and bringing overseas drugs and innovations into the Chinese mainland, while helping mainland enterprises to go global,” says Bernard Cheung, CEO of GBAICTI.
He notes that clinical data on Chinese people, such as dosage and efficacy, are still underrepresented in developing drugs as many international drugmakers are based in the West. It’s also necessary for southern China to have a regional clinical trial pivot, given the growing demand for medical innovation.
Cross-border synergy
An example of regional synergy is an ongoing clinical trial for ICVAX — a therapeutical human immunodeficiency virus vaccine developed by HKU. The vaccine aims to achieve a functional cure for HIV that attacks the body’s immune system, by inducing sustained T-cell immunity, keeping the virus undetectable in the blood in the long term.
Since the first case of Acquired Immuno Deficiency Syndrome was diagnosed in 1981, more than 40 million people have died from the disease. Today, more than 39 million people are living with HIV. While antiretroviral therapy can suppress the virus, AIDS remains incurable.
The first-in-human first-phase clinical trial using ICVAX, performed at Shenzhen Third People’s Hospital in 2024, recruited 45 patients. The test met its goals of evaluating the therapy’s safety, maximum tolerated dose and immunogenicity in stable HIV-1 patients, with the virus suppressed by antiretroviral therapy.
Cheung says a successful vaccine would benefit patients worldwide, especially in regions hard hit by the virus, such as Africa and countries involved in the Belt and Road Initiative.
In July last year, GBAICTI, BAY TRIAL and Immuno Cure BioTech — a clinical-stage biotechnology company holding the exclusive license for the vaccine’s patent — jointly signed a memorandum of understanding on the first-ever cross-boundary multi-center second-phase trial of ICVAX.
The exercise will recruit 350 AIDS patients from cities including Hong Kong, Shenzhen, Guangzhou and Beijing. Among them, 110 will receive placebos, while the others will get four doses of ICVAX at medium and low levels, followed by a booster every six months.
The second phase will look for early signs of the vaccine’s effectiveness. If successful, a large-scale third stage would follow to confirm its efficacy that is expected to result in the drug being approved for market use.
The GBAICTI network offers a one-stop platform for drugmakers hoping to conduct clinical trials on the mainland, and speeds up the process by identifying the most suitable investigators. A key facility of GBAICTI, the Real-World Study & Application Centre, set up on Dec 22 last year, supports this with its database to locate patients with specific diseases.
“We are trying to facilitate the cross-boundary flow of biological samples. The minimum option is to allow an eased flow of such samples within the Hetao zone, if not a full scale cross-boundary flow between the two places,” says Cheung.
Biological samples need smooth cross-boundary transport within a short period of time, involving multiple authorities and requiring close coordination, he says, adding that both sides are now testing the process through pilot projects to ensure a smooth flow between locations.
Cross-boundary flow of bio-samples in the Hetao zone would let Hong Kong access rare disease DNA for research and development, supporting its goal to become a global clinical trial hub, says Kenny Shui, vice-president of Our Hong Kong Foundation and executive director of the Public Policy Institute.
He suggests creating a white list for institutions and biomedical enterprises to enable simplified Customs clearance of blood and cell samples for certified institutions at Hetao. This would help Hong Kong combine cross-boundary advantages and support its goal of becoming a global biomedical innovation center.
Cheung says drugmakers and research institutes should set up a central lab in the Hetao zone. Within Hong Kong Park, a biobank managed by the Hospital Authority and the Chinese University of Hong Kong, stores up to 400,000 samples, including tissues, blood, cells and DNA. Several hospitals have already deposited samples. The biobank operates like a library, with samples accessible to other parties under reasonable conditions and reviewed by a judging panel.
According to Cheung, Hong Kong and the mainland’s Greater Bay Area cities are discussing ways to speed up ethics reviews, such as standardizing paperwork, using electronic applications, and holding more frequent board meetings. He hopes the process will, one day, be as simple as filling out an arrival card, where the required information is similar even if formats differ.
To further expedite the process, Shui says an ethics review platform could be set up, with approval by one board being recognized by the others.
In March 2024, the Hong Kong authorities consolidated all hospital cluster ethics committees into the Hospital Authority Central Institutional Review Board. It has since processed over 1,000 applications, cutting the approval time frame period from between four and eight months to 30 days for general cases and two months for complex ones.
Boosting trials, bridging gaps
Noting that the recent policy relaxations at home are aimed at speeding up clinical trials, Shui says it could boost the number in Hong Kong which, currently, is about 300 annually, mostly conducted by the two medical schools. Cheung proposes getting more HA hospitals and clinics involved, and partnering with experts and hospitals in the Greater Bay Area to maximize results.
Policy bottlenecks aside, a talent shortage is holding back the development of clinical trials in Hong Kong, says Shui. The city has top-tier investigators, but lacks supporting staff like clinical research coordinators and nurses. He believes a qualifications framework with a clear career path — from coordinator to project manager — would attract young talent. The system should align with international standards and be mutually recognized with the mainland, especially in the Greater Bay Area, so that local talent can understand global and mainland practices.
GBAICTI will launch the International Clinical Trial Academy next year to train professionals in the region through seminars, conferences and workshops. The focus will be on medical professionals needing clinical trial knowledge, and clinical trial coordinators who support doctors and monitor studies.
While local universities like HKU and CUHK offer related programs, Cheung says GBAICTI aims to provide structured, continuous training, moving beyond on-the-job learning. The training, geared to attracting participants from other cities in the region, will be conducted in English to align with international clinical trial standards.
According to a 2025 TF Securities report, China has led globally in the number of innovative drugs produced since 2020 — rising from 38 in 2015 to 704 in 2024. The number of drug out-licensing deals has also surged, reaching 157 worth $136 billion in 2025 — up from 94 worth $51.9 billion the year before.
The mainland’s biotechnology growth has benefited Hong Kong which, leveraging its financial strengths, has become the world’s second-largest biotech fundraising hub. Shui says this makes Hong Kong well-placed to help mainland drugmakers go global by offering clinical trials that meet international standards and encouraging them to register new drugs and set up regional headquarters in the SAR.
With Hong Kong’s common law system and strong intellectual property rights that are aligned with global norms, the city provides a safe base for managing global patent strategies and reducing legal risks like patent disputes abroad. In this way, it can serve as both a “superconnector” and “super value-adder”, acting as a launchpad for mainland innovations eyeing the global market, says Shui.
ALSO READ: China’s battle against rare diseases gets pat on the back
The HKSAR government plans to set up the Hong Kong Centre for Medical Products Regulation later this year, with full implementation of “primary evaluation” by 2030. Under the “1+” mechanism introduced in November 2023, drug registration now requires approval from only one, instead of two, nonlocal regulators. As of last month, 19 drugs had been registered under this mechanism.
Hong Kong also lacks talent for independent assessment of raw clinical data — a key barrier to achieving primary evaluation for new drug registrations — says Shui. He suggests the city recruit experienced reviewers from agencies like China’s National Medical Products Administration and the United States’ Food and Drug Administration with competitive pay to form CMPR’s core team, and join local universities in offering training and career pathways for drug and medical device reviewers with market-driven salaries.
The “1+” mechanism has boosted business incentives for clinical trials, while the planned free flow of bio-samples in Hetao will further strengthen Hong Kong’s appeal, says Shui.
Contact the writer at stushadow@chinadailyhk.com